Article
ASCO 2019: Results from the Phase 3 KEYNOTE-048 Trial
The Educated Patient®: Research Updates provides current clinical updates for different disease states. The following information is for educational purposes and is not medical advice.
FOR YOUR REFERENCE: What Are Clinical Trials?
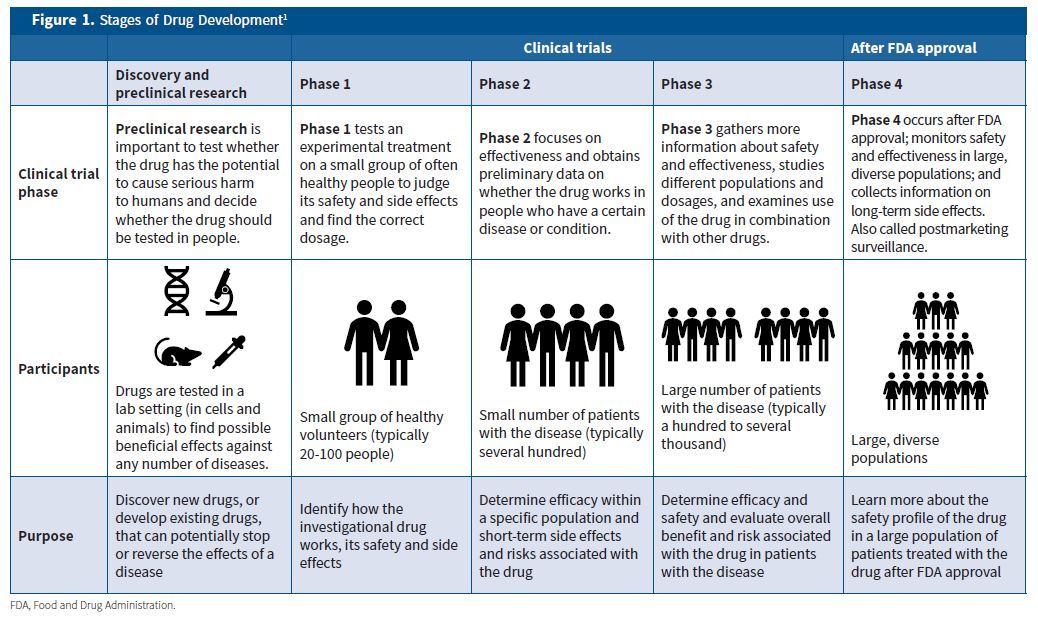
Clinical trials determine whether a drug works in humans and if it is safe and effective. To find out whether a drug can be approved for use, the Food and Drug Administration (FDA) requires four phases of a clinical trial. The number of participants increases in each phase, starting from 20 to
80 people for a phase 1 trial to up to 3,000 for a phase 3 trial (Figure 1).1
- Phase 1: tests an experimental treatment on a small group of often healthy people to judge its safety and side effects and find the correct dosage.
- Phase 2: focuses on effectiveness and obtains preliminary data on whether the drug works in people who have a certain disease or condition.
- Phase 3: gathers more information about safety and effectiveness, studies different populations and dosages, and examines use of the drug in combination with other drugs.
- Phase 4: occurs after FDA approval; monitors safety and effectiveness in large, diverse populations; and collects information on long-term side effects.
FOR YOUR REFERENCE: What Is Head and Neck Squamous Cell Carcinoma?
Cancers of the head and neck typically begin in the squamous cells that line the inside of the mouth, nose, and throat. Head and neck squamous cell carcinoma (HNSCC) includes cancers of the oral cavity, pharynx, larynx, paranasal sinuses, nasal cavity and the salivary glands.2 They are the most common malignancies that occur in the head and neck.3
Tumors that arise in the oropharynx, the part of the throat just behind the oral cavity, are increasingly associated with prior infection with oncogenic strains of human papillomavirus (HPV). HNSCCs of the larynx and oral cavity are still primarily linked to smoking and are now collectively referred to as HPV-negative HNSCC.3
Because no screening strategy has proved effective, careful physical examination remains the primary approach for early detection of HNSCC. Risk factors for HNSCC include alcohol and tobacco use, exposure to environmental pollutants, and infection with viral disease such as HPV and Epstein-Barr virus.3
Early-stage cancers of the oral cavity may be treated with surgery alone, and larynx cancers may be treated with surgery and radiation. Other HNSCCs usually require a combination of surgery, chemotherapy, radiation therapy and targeted therapy. Treatment of HNSCC that has spread to other parts of the body (metastatic) may include immunotherapy and palliative care to relieve symptoms and side effects.4
FOR YOUR REFERENCE: What Medications Were Investigated in the KEYNOTE-048 Trial?
Keytruda (pembrolizumab) is a type of immunotherapy called a monoclonal antibody. It is designed to prevent cancer cells from multiplying and spreading inside the body and is approved by the FDA for several types of cancer, including metastatic or unresectable (not removable by surgery) HNSCC.5,6
To understand how Keytruda works, it helps to first learn about two cell proteins called programmed cell death protein 1 (PD-1) and programmed death-ligand 1 (PD-L1). PD-1 is found on the body’s T cells, a type of immune cell that normally attacks and kills invaders such as cancer cells. PD-L1 is found on cancer cells as well as other types of cells. If PD-1 and PD-L1 bond together, this interaction stops T cells from killing cancer cells and allows the cancer to spread. Keytruda prevents PD-1 and PD-L1 from bonding, freeing T cells to continue killing cancer cells.7
Erbitux (cetuximab) is an epidermal growth factor receptor (EGFR) inhibitor that is designed to block the activity of the EGFR receptor. EGFR receptors are found on the surface of normal cells and tumor cells and they are important for the control of cell growth. By blocking EGFR activity on head and neck cancer cells, Erbitux may stop those cancer cells from growing.8
5-fluorouracil (5-FU) is a type of chemotherapy used to prevent cell proliferation.9 Cisplatin and carboplatin are platinum-based chemotherapy medications.10,11
ASCO 2019: Phase 3 KEYNOTE-048 Trial
The phase 3 KEYNOTE-048 trial aimed to determine whether Keytruda alone or in combination with platinum-based chemotherapy improves overall survival (OS) compared with Erbitux plus platinum-based chemotherapy in participants with previously untreated recurrent or metastatic HNSCC that is not able to be cured by local therapies.12
Patients were divided into groups based on percentage of PD-L1-expressing tumor cells (or combined positive score [CPS]), HPV status according to p16 immunohistochemistry status for oropharyngeal cancers (positive or negative) and Eastern Cooperative Oncology Group performance status, then randomly assigned to receive one of the following treatments12: Keytruda alone, Keytruda combined with platinum-based chemotherapy (carboplatin or cisplatin, and 5-FU) or Erbitux plus platinum-based chemotherapy (carboplatin or cisplatin, and 5-FU). Participants received all treatments intravenously.12
OS and progression-free survival (PFS) were primary end points.2 Secondary end points included safety and tolerability and proportion of participants with objective response (complete or partial).12
Results
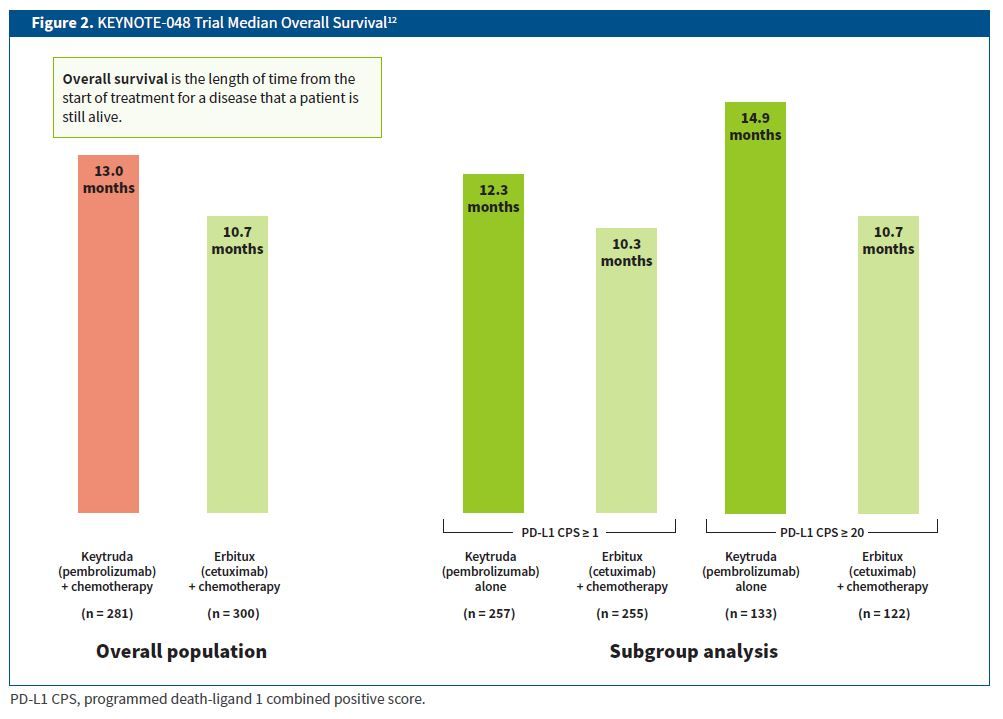
The results of the trial demonstrated significant improvements in OS as follows (Figure 2)12:
- In the overall population, patients who received Keytruda plus chemotherapy had a median OS of 13.0 months compared with 10.7 months in patients who received Erbitux plus chemotherapy.
- In the subgroup analysis of patients grouped by PD-L1 CPS, the median OS was as follows12:
- Patients with PD-L1 CPS of 20 or greater: 14.9 months for the Keytruda alone group and 10.7 months for the Erbitux plus platinum-based chemotherapy group.
- Patients with PD-L1 CPS of 1 or greater: 12.3 months for the Keytruda group and 10.3 months for the Erbitux plus chemotherapy group.
Neither PFS nor objective response for either the Keytruda alone or Keytruda plus platinum-based chemotherapy group showed significant improvement compared with the Erbitux plus chemotherapy group in any population.12
The most common side effects reported in patients who received Keytruda alone were anemia and fatigue. Keytruda in combination with platinum-based chemotherapy was associated with a greater risk of anemia, cough and hypothyroidism than Erbitux plus platinum-based chemotherapy.12
KEYNOTE-048 findings support the use of Keytruda alone and combined with platinum-based chemotherapy as a new first-line standard of care for recurrent or metastatic HNSCC that is not able to be cured by local therapies.12,13 Based on the KEYNOTE-048 study findings, Keytruda was approved by the FDA for first-line treatment of HNSCC in combination with platinum-based chemotherapy for all patients and as a single medication for patients whose tumors express PD-L1 with a CPS of 1 or greater.6
Not all patients qualify for certain clinical trials. If you are interested in enrolling in a trial, talk with your doctor about which treatment options would be most appropriate for you.
FOR YOUR REFERENCE: Glossary of Terms
Anemia: a condition where the body doesn’t have enough heathy red blood cells to carry sufficient oxygen to the body’s tissues
Cell proliferation: an increase in the number of cells as a result of cell growth and cell division
Chemotherapy: treatment that uses drugs to stop the growth of cancer cells by either killing the cells or stopping them from dividing. These drugs are taken by mouth or injected and enter the bloodstream so they can help fight cancers throughout the body. This can affect cancer cells and normal cells.
Combined positive score (CPS): measure of the number of PD-L1-positive cells (tumor cells, lymphocytes, macrophages) divided by the total number of viable tumor cells, multiplied by 100
Eastern Cooperative Oncology Group (ECOG) performance status: scales and criteria used by doctors and researchers to assess disease progression and how the disease affects the patient’s daily living abilities, as well as determine appropriate treatment and prognosis
Efficacy: the ability to produce a desired outcome. In the case of cancer treatments, the desired outcome is a decrease in the number of cancer cells or the disappearance of cancer cells.
End point: the main result that is measured at the end of a study to see if a given treatment worked
Epidermal growth factor receptor (EGFR): a protein on the surface of cells that normally helps the cells grow and divide. Sometimes cancer cells have too much EGFR, which makes them grow faster.
Epidermal growth factor receptor (EGFR) inhibitors: a drug that blocks the signal from EGFR that tells the cells to grow. Some of these drugs can be used to treat cancer.
Epstein-Barr virus (EBV): also known as human herpesvirus 4, a member of the herpes virus family. It is one of the most common human viruses and spreads mainly through bodily fluids, primarily saliva. Most people will get infected with EBV at some point.
First-line therapy: the first treatment given for a disease
Human papillomavirus (HPV): a common sexually transmitted infection
Hypopharynx: the lower part of the throat (pharynx) that lies right behind the larynx
Hypothyroidism: when the thyroid gland does not produce enough hormone, which causes a person to slow down, feel tired and gain weight
Immunohistochemistry: method used to detect the presence of a specific protein marker that can assist with accurate tumor classification and diagnosis
Immunotherapy: a type of therapy that uses substances to stimulate or suppress the immune system to help the body fight cancer, infection and other diseases
Larynx: also called the voice box; a short passageway formed by cartilage just below the pharynx in the neck. The larynx contains the vocal cords and has a small piece of tissue, called the epiglottis, which moves to cover the larynx to prevent food from entering the air passages.
Malignancy: a disease in which abnormal cells divide in an uncontrolled way and can invade nearby tissues and spread to other parts of the body
Metastatic: cancer that has spread from the location where it was initially found or diagnosed to other parts of the body
Monoclonal antibody: a type of protein made in the laboratory that can bind to substances in the body, including cancer cells
Nasal cavity: the space inside the nose above the bone that forms the roof of the mouth; this space curves down at the back to join the throat
Objective response rate: a specific percentage of patients who responded to treatment and their tumors completely or partially shrunk (complete response or partial response)
Oncogenic: cancer-causing
Oral cavity: the mouth, including the lips, the lining inside the cheeks and lips, the front two-thirds of the tongue, the gums, the floor and roof of the mouth, and the area behind the wisdom teeth
Oropharynx: the middle part of the throat (pharynx) just beyond
the mouth
Overall survival (OS): the length of time from either the date of diagnosis or the start of treatment for a disease that a patient is still alive
p16: a tumor suppressor gene. Overexpression of p16 is considered a surrogate marker of oncogenic human papillomavirus infection and correlates with a good prognosis in head and neck squamous cell carcinoma.
Palliative: a type of medical care given to improve the quality of life for patients who have a serious or life-threatening disease
Paranasal sinuses: a group of four paired air-filled spaces that surround the nasal cavity
Programmed death 1 (PD-1): a protein on the surface of T cells that helps keep the body’s immune responses in check
Programmed death-ligand 1 (PD-L1): a protein found on some types of cancer cells
Programmed death-ligand 1 (PD-L1) combined positive score (CPS): a measure of the number of PD-L1-positive cells divided by the total number of tumor cells found. PD-L1 protein expression in HNSCC is determined by using CPS. Tumors have PD-L1 expression if CPS ≥ 1. Tumors that express higher amounts of PD-L1 may respond particularly well to checkpoint inhibitors (a type of immunotherapy drug), like Keytruda.
Pharynx: the hollow tube inside the neck that starts behind the nose and ends at the top of the trachea (windpipe) and the esophagus (the tube that goes to the stomach)
Platinum-based chemotherapy: anticancer drugs, such as cisplatin and carboplatin, that contain the metal platinum. Although effective, they have side effects that limit their use.
Primary end point: the main result that is measured at the end of a study to see if a given treatment worked
Progression-free survival (PFS): the length of time during and after the treatment of a disease that a patient lives with the disease but it does not get worse
Radiation therapy: type of cancer treatment that uses beams of intense energy to kill cancer cells
Recurrent: cancer that returns after treatment
Salivary glands: exocrine glands in the mouth that produce saliva and release it into the mouth via ducts
Secondary endpoint: measures other relevant questions in a study
Squamous cells: cells found in the outer layer of skin and in the mucous membranes, which are the moist tissues that line body cavities such as the airways and intestines. Head and neck squamous cell carcinoma develops in the mucous membranes of the mouth, nose and throat.
Subgroup analysis: a group of persons in a trial identified by a specific trait, such as gender, race or HPV status, that is studied in order to determine if people with that trait are affected by the treatment
Systemic therapy: treatment using substances that travel through the bloodstream, reaching and affecting cells all over the body
T cell: a type of white blood cell that is part of the immune system; these cells protect the body from infection and may help fight cancer
Toxicity: the extent to which something is poisonous or harmful
References
- What are clinical trials and studies? National Institute on Aging. Accessed May 13, 2021. https://www.nia.nih.gov/health/what-are-clinical-trials-and-studies
- Head and neck cancers. National Cancer Institute. Updated March 29, 2017. Accessed May 20, 2021. https://www.cancer.gov/types/head-and-neck/head-neck-fact-sheet
- Johnson DE, Burtness B, Leemans CR, Lui VWY, Bauman JE, Grandis JR. Head and neck squamous cell carcinoma. Nature Reviews Disease Primers. 2020;6(1):92. doi:10.1038/s41572-020-00224-3
- Head and neck cancers: types of treatment. American Society of Clinical Oncology. Accessed May 21 2021. https://www.cancer.net/cancer-types/head-and-neck-cancer/types-treatment
- How does Keytruda work? Merck Oncology. Accessed May 1, 2021. keytruda.com/how-does-keytruda-work
- FDA approves pembrolizumab for first-line treatment of head and neck squamous cell carcinoma. Food and Drug Administration. Accessed May 21, 2021. https://www.fda.gov/drugs/resources-information-approved-drugs/fda-approves-pembrolizumab-first-line-treatment-head-and-neck-squamous-cell-carcinoma
- Prasad V, Kaestner V. Nivolumab and pembrolizumab: Monoclonal antibodies against programmed cell death-1 (PD-1) that are interchangeable. Semin Oncol. 2017;44(2):132-135. doi:10.1053/j.seminoncol.2017.06.007
- ERBITUX (cetuximab). Prescribing information. ImClone LLC; 2021. Accessed August 2, 2021. https://uspl.lilly.com/erbitux/erbitux.html#pi
- Wigmore PM, Mustafa S, El-Beltagy M, Lyons L, Umka J, Bennett G. Effects of 5-FU. Adv Exp Med Biol. 2010;678:157-164. doi:10.1007/978-1-4419-6306-2_20
- Cisplatin prescribing information. WG Critical Care, LLC; 2019. Accessed May 20, 2021. https://www.accessdata.fda.gov/drugsatfda_docs/label/2019/018057s089lbl.pdf
- Paraplatin (carboplatin) injection prescribing information. Bristol-Myers Squibb Company; 2021. Accessed May 21, 2021. https://www.accessdata.fda.gov/drugsatfda_docs/label/2010/020452s005lbl.pdf
- Burtness B, Harrington KJ, Greil R, et al. Pembrolizumab alone or with chemotherapy versus cetuximab with chemotherapy for recurrent or metastatic squamous cell carcinoma of the head and neck (KEYNOTE-048): a randomised, open-label, phase 3 study. Lancet. 2019;394(10212):1915-1928. doi:10.1016/S0140-6736(19)32591-7
- Rischin D, Harrington KJ, Greil R, et al. Protocol-specified final analysis of the phase 3 KEYNOTE-048 trial of pembrolizumab (pembro) as first-line therapy for recurrent/metastatic head and neck squamous cell carcinoma (R/M HNSCC). J Clin Oncol. 2019;37(15):6000. doi:10.1200/JCO.2019.37.15_suppl.6000