- Winter 2018
- Volume 6
- Issue 1
How One Person Beat Cancer by Participating in a Clinical Trial
After being diagnosed with glioblastoma, experimental immunotherapy saved his life.
IN THE FALL OF 2009, I was recruited to play baseball at Holy Cross College in Notre Dame, Indiana. But a couple of years in, things began to change. My attitude shifted; I became both disinterested and irritable. I lost my sense of humor, and my personal relationships suffered. Within six months, I quit the baseball team, and then flunked out of school. In no time, it seemed, I lost everything I had worked so hard for.
After I left school, my parents forced me to see a therapist to check for depression. My personality changes made no sense to me, and I resisted being treated for a mental illness. I got a job at a factory and watched from home as my friends graduated and started their careers.
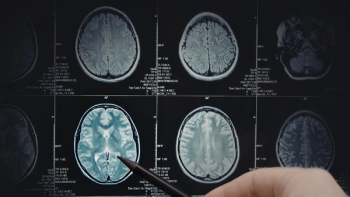
Later, when the headaches started, my doctor wasn’t overly concerned. After all, it was a stressful time in my life — headaches would be a natural physical reaction. Eventually, when my vision was affected and I began experiencing partial paralysis, it was clear something was wrong. After a CT scan revealed a golf ball-size tumor on my brain, I was rushed into surgery. A week later, I was diagnosed with glioblastoma, an aggressive form of brain cancer that was lethal in nearly every case. I had, at most, six months to live. I was 22.
My oncologist recommended that I immediately begin chemotherapy and radiation, measures that might prolong my life for a while. My parents actually told this doctor — a really good doctor who wanted to start treatment immediately — that they needed time to process and look at alternatives.
Taking time off work, my parents began the tough task of researching any hospital or clinical team that was investigating my type of cancer. They weren’t looking for more time; they wanted a cure. They worked the phones — Duke, Miami, a host of other places — before choosing the University of Michigan (U-M). Its Brain Tumor Program had a promising clinical trial.
With my oncologist’s approval, I underwent grueling tests to see if I was a suitable candidate for the trial. I was accepted into DCVax, an immunotherapy treatment program that used my own cells to fight the cancer and keep it away forever.
For two years, my oncologist worked alongside my clinical trial team at U-M. After every treatment and every surgery, reports and emails were exchanged to bring each other up to speed on my progress. The immunotherapy and six surgeries were done at U-M, and my chemotherapy and radiation were done near my home. The process worked well — so well that when I made it to the end of the clinical trial, no one quite knew what to do next. People rarely survived this, and yet my tumor was gone. The clinical trial worked exactly the way the doctors intended.
Now, five years later, I am officially cancer-free and a college graduate. My doctors aren’t as worried anymore about recurrence. I will soon be working full time with Riverbend Cancer Services in South Bend, Indiana, to help clients locate alternative cancer treatments around the country.
Articles in this issue
almost 8 years ago
Book Corneralmost 8 years ago
Establishing a Safe Harbor for Survivorsalmost 8 years ago
Think Twice About Friending Your Nurse on Social Mediaalmost 8 years ago
The Quest to End Survivor Pain