ASCO 2020: Results from the Phase 3 KEYNOTE-604 Trial
The Educated Patient®: Research Updates provides current clinical updates for different disease states. The following information is for educational purposes and is not medical advice.
FOR YOUR REFERENCE: What Are Clinical Trials?
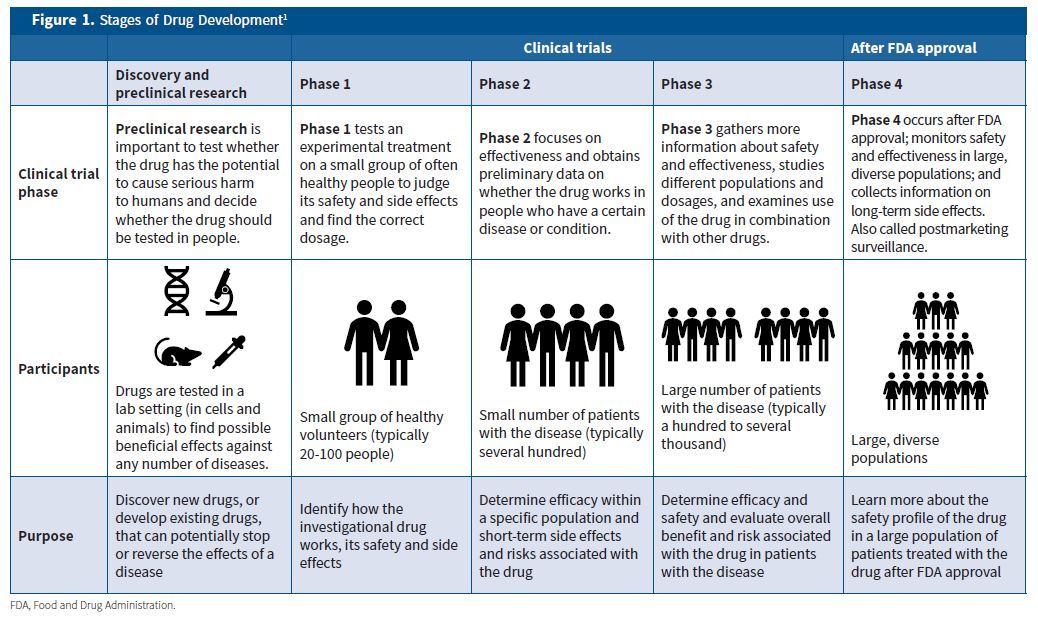
Clinical trials determine whether a drug works in humans and if it is safe and effective. To find out whether a drug can be approved for use, the Food and Drug Administration (FDA) requires four phases of a clinical trial. The number of participants increases in each phase, starting from 20 to 80 people for a phase 1 trial to up to 3,000 for a phase 3 trial (Figure 1).1
- Phase 1: tests an experimental treatment on a small group of often healthy people to judge its safety and side effects and find the correct dosage.
- Phase 2: focuses on effectiveness and obtains preliminary data on whether the drug works in people who have a certain disease or condition.
- Phase 3: gathers more information about safety and effectiveness, studies different populations and dosages, and examines use of the drug in combination with other drugs.
- Phase 4: occurs after FDA approval; monitors safety and effectiveness in large, diverse populations; and collects information on long-term side effects.
FOR YOUR REFERENCE: What Is Extensive-Stage Small Cell Lung Cancer?
About 10% to 15% of all lung cancers are small cell lung cancer (SCLC), also called oat cell cancer. Because SCLC tends to grow and spread faster than non-small cell lung cancer, about 70% of people will have cancer that has already spread at the time they receive a diagnosis.2 SCLC is considered extensive stage (ES) when it has spread widely throughout the lung, to the other lung, to lymph nodes on the other side of the chest or to other parts of the body, including the bone marrow. SCLC that has spread to the fluid around the lung is also considered to be ES by many doctors.3 Smoking is the leading risk factor for lung cancer. An estimated 80% of lung cancer deaths result from smoking, although this percentage is probably higher for SCLC. It is rare for someone who has never smoked to have SCLC.4
The most common symptoms of lung cancer include persistent coughing; coughing up blood or rust-colored phlegm; chest pain that is often worse with deep breathing, coughing or laughing; hoarseness; loss of appetite; unexplained weight loss; shortness of breath; fatigue; infections, such as bronchitis and pneumonia, that persist or recur; and new onset of wheezing.3
ES-SCLC is cancer that has spread too far for surgery or radiation therapy to be useful as the initial treatment. For patients with ES-SCLC, chemotherapy, possibly combined with an immunotherapy drug, is typically the first treatment option.5 Other treatment options include5:
- Radiation to the chest or brain (to prevent progression in this area), or to relieve symptoms if the cancer has spread to the bones, brain or spinal cord.
- Lower-dose chemotherapy or palliative/supportive care.
- Clinical trials of new chemotherapy drugs and drug combinations.
FOR YOUR REFERENCE: What Medications Were Investigated in the KEYNOTE-604 Trial?
Keytruda (pembrolizumab) is a type of immunotherapy called a monoclonal antibody. It is designed to prevent cancer cells from multiplying inside the body.6 To understand how Keytruda works, it helps to first learn about two cell proteins called programmed cell death 1 (PD-1) and programmed death-ligand 1 (PD-L1). PD-1 is found on the body’s T cells, a type of immune cell that normally attacks and kills invaders such as cancer cells. PD-L1 is found on cancer cells as well as other cells. If PD-1 and PD-L1 bond together, this interaction stops the T cells from killing cancer cells and allows them to spread. Keytruda prevents PD-1 and PD-L1 from bonding, enabling T cells to continue killing cancer cells.7
In 2019, the FDA granted accelerated approval to pembrolizumab for the treatment of patients with metastatic SCLC with disease progression on or after platinum-based chemotherapy and at least one other prior line of therapy. Per the FDA, approval would be continued only if the results of a clinical trial showed significant OS benefit with pembrolizumab. The indication was withdrawn in March 2021, as phase 3 trial results did not meet the overall survival (OS) requirements for continued indication approval.8
Toposar (etoposide), also commonly known as VP-16, is a chemotherapy drug indicated in combination with other approved chemotherapeutic agents as first-line treatment in patients with SCLC.9 The most commonly used combination of chemotherapy drugs is etoposide plus either cisplatin or carboplatin, which are platinum-based chemotherapy drugs.5
ASCO 2020: Phase 3 KEYNOTE-604 Trial
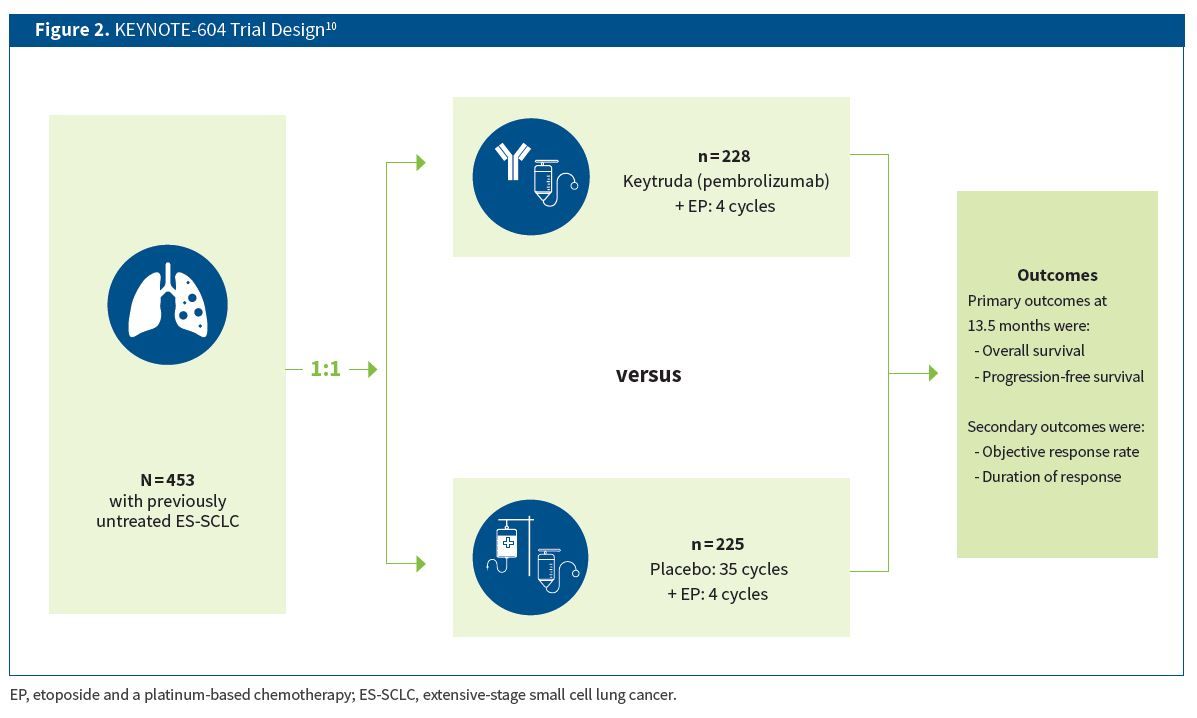
The phase 3 KEYNOTE-604 clinical trial assessed the efficacy of Keytruda plus etoposide and a platinum-based chemotherapy (EP) compared with placebo plus EP for the treatment of ES-SCLC in the first-line setting, meaning in those who have not received prior treatment for their disease. Patients (N = 453) with previously untreated ES-SCLC and no untreated central nervous system (CNS) metastases were randomly assigned to receive either Keytruda or saline placebo for up to 35 cycles plus four cycles of standard-dose EP containing cisplatin or carboplatin with a median follow up of 13.5 months (Figure 2).10 Primary end points were OS and progression-free survival (PFS) in the intention-to-treat population. Objective response rate (ORR) and duration of response (DOR) were secondary end points in the trial.10
Results
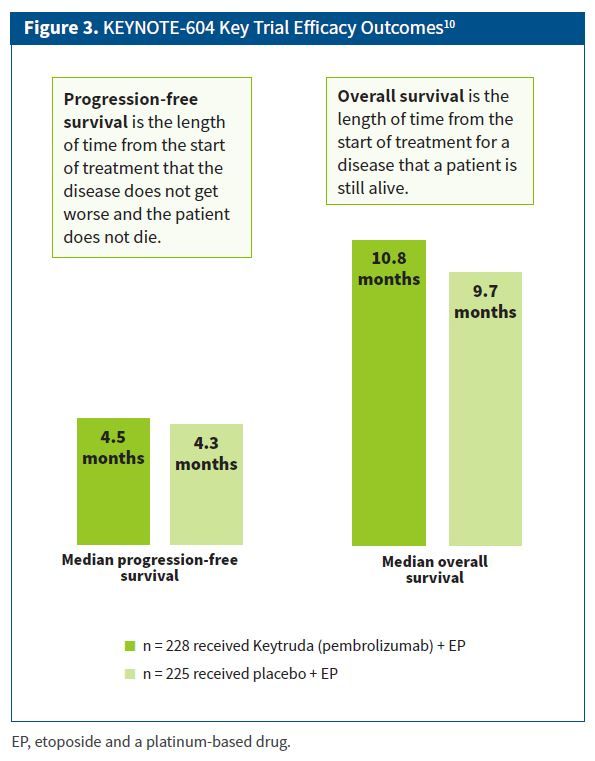
By the second interim analysis at approximately 22 months after the study start, the combination of Keytruda plus EP significantly improved PFS (median 4.5 months) compared with placebo plus EP (median 4.3 months; Figure 3).10 At the final analysis, approximately 31 months after the study start, the median OS was prolonged in the Keytruda plus EP group (10.8 months) compared with the placebo plus EP group (9.7 months), although statistical significance was not reached at the final analysis. ORR at final analysis was 70.6% for Keytruda plus EP compared with 61.8% for placebo plus EP. Median DOR was 4.2 months in the Keytruda plus EP group compared with 3.7 months in placebo plus EP group. No unexpected toxicities were observed, and side effects were consistent with those observed with Keytruda alone in patients with SCLC.10
Investigators determined that first-line treatment with Keytruda plus EP significantly improved PFS and prolonged OS without unexpected toxicities. The results of this study confirmed the benefits of Keytruda-containing regimens for ES-SCLC. However, the difference in OS was not significant. The indication for the treatment of patients with metastatic SCLC with disease progression on or after platinum-based chemotherapy and at least one other prior line of therapy was withdrawn in March 2021, as phase 3 trial results did not meet the OS requirements for continued indication approval.8,11
Not all patients qualify for certain clinical trials. If you are interested in enrolling in a trial, talk with your doctor about which treatment options would be most appropriate for you.
FOR YOUR REFERENCE: Glossary of Terms
Bone marrow: the soft, inner part of some bones; made up of fatty tissue or blood-forming cells that create new red and white blood cells and blood platelets. Some cancers first develop in the bone marrow.
Bronchitis: a short-lived or long-lasting (and often recurring) inflammation of the main air passages to the lungs; occurs because of a virus or inhaled irritant
Central nervous system (CNS) metastasis: cancer that has spread from the original (primary) tumor to the central nervous system (ie, the brain and spinal cord)
Chemotherapy: treatment that uses drugs to stop the growth of cancer cells either by either killing the cells or stopping them from dividing. These drugs are taken by mouth or injected and enter the bloodstream so they can help fight cancers that spread throughout the body. This can affect cancer cells and normal cells.
Duration of response (DOR): the length of time from first evidence of the tumors being partially or completely shrunk (partial response or complete response) to disease progression or death
Efficacy: the ability to produce a desired outcome. In the case of cancer treatments, the desired outcome is a decrease in the number of cancer cells or the disappearance of cancer cells.
Extensive-stage lung cancer: cancer that has spread widely throughout the lung, to the other lung, to lymph nodes on the other side of the chest or to other parts of the body, including the bone marrow. Small cell lung cancer that has spread to the fluid around the lung is extensive stage as well.
First-line treatment: the first treatment given for a disease
Immune cell: a cell that’s part of the immune system and helps fight infections and diseases
Immunotherapy: type of therapy that uses substances to stimulate or suppress the immune system to help the body fight cancer, infection and other diseases. Some types of immunotherapy target only certain cells of the immune system; others affect the immune system in a general way.
Intention to treat (ITT): analysis of the results of an experiment, based on the initial treatment assignment and not on the treatment eventually received
Lymph nodes: part of the lymphatic system in the body’s immune system; carry fluid containing white blood cells, which help fight infections
Metastatic: cancer that spreads from its original location to other, distant parts of the body
Monoclonal antibody: a type of protein made in the laboratory that can bind to substances in the body, including cancer cells
Non-small cell lung cancer (NSCLC): type of cancer affecting the lung; about 80% to 85% of lung cancers. The main subtypes are adenocarcinoma, squamous cell carcinoma, and large cell carcinoma and are grouped as NSCLC because their treatment and outlook are similar even though they start in different types of lung cells.
Oat cell cancer: another name for small cell lung cancer because the cells look like oats under a microscope
Objective response rate (ORR): a specific percentage of patients who responded to treatment and their tumors completely or partially shrunk (complete response or partial response)
Overall survival (OS): the length of time from either the date
of diagnosis or the start of treatment for a disease that a patient is
still alive
Palliative: medical care given to improve the quality of life for patients who have a serious or life-threatening disease
Placebo: an inactive substance or other intervention that looks the same and is given the same way as an active drug or treatment being tested. The effects of the active drug or other intervention are compared with the effects of the placebo.
Platinum-based chemotherapy: anticancer drugs, such as cisplatin and carboplatin, that contain the metal platinum. Although effective, they have side effects that limit their use.
Pneumonia: a lung infection leading to difficulty breathing and fluid in the lungs
Primary end point: the main result that is measured at the end of a study to see if a given treatment worked
Programmed cell death 1 (PD-1): a protein on the surface of T cells that helps keep the body’s immune responses in check
Programmed cell death 1 (PD-1) inhibitor: a drug that blocks PD-1, thereby boosting the immune response against cancer cells. This can shrink some tumors or slow their growth.
Programmed death-ligand 1 (PD-L1): a protein found on some types of cancer cells
Progression-free survival (PFS): the length of time during and after the treatment of a disease that a patient lives with the disease but it does not get worse
Radiation therapy: type of cancer treatment that uses beams of intense energy to kill cancer cells
Secondary end point: additional results of interest that the study is not specifically powered to assess
Side effect: any unfavorable or unintended disease, sign or symptom that occurs during the time a patient is receiving a medical treatment or procedure
Small cell lung cancer: a fast-growing and spreading cancer that, in 70% of cases, has already spread by the time a patient receives a diagnosis
Statistical significance: a mathematical measure of difference between groups. The difference is statistically significant if it is greater than what might be expected to happen by chance alone.
Supportive care: the prevention and management of the physical
and psychological side effects of cancer and its treatment
T cell: a type of white blood cell; part of the immune system developed from stem cells in the bone marrow. T cells help protect the body from infection and may help fight cancer.
Toxicity: the extent to which something is poisonous or harmful
Wheezing: a whistling or rattling sound in the chest made while breathing in or out; associated with difficulty breathing
References
- What are clinical trials and studies? National Institute on Aging. Accessed May 13, 2021. https://www.nia.nih.gov/health/what-are-clinical-trials-and-studies
- About lung cancer. American Cancer Society. Updated October 1, 2019. Accessed May 11, 2021. https://www.cancer.org/content/dam/CRC/PDF/Public/8703.00.pdf
- Lung cancer early detection, diagnosis, and staging. American Cancer Society. Updated April 22, 2021. Accessed May 11, 2021. https://www.cancer.org/content/dam/CRC/PDF/Public/8705.00.pdf
- Small cell lung cancer causes, risk factors, and prevention. American Cancer Society. Updated May 16, 2016. Accessed May 11, 2021. https://www.cancer.org/content/dam/CRC/PDF/Public/8709.00.pdf
- Treating small cell lung cancer. American Cancer Society. Updated March 3, 2021. Accessed May 14, 2021. https://www.cancer.org/content/dam/CRC/PDF/Public/8711.00.pdf
- How Keytruda works. Merck Oncology. Accessed May 1, 2021. https://www.keytruda.com/how-does-keytruda-work/
- Prasad V, Kaestner V. Nivolumab and pembrolizumab: monoclonal antibodies against programmed cell death-1 (PD-1) that are interchangeable. Semin Oncol. 2017;44(2):132-135. doi:10.1053/j.seminoncol.2017.06.007
- Merck provides update on Keytruda (pembrolizumab) indication in metastatic small cell lung cancer in the US. News release. Merck & Co, Inc. March 1, 2021. Accessed May 13, 2021. https://s2.q4cdn.com/584635680/files/doc_news/Merck-Provides-Update-on-KEYTRUDA-pembrolizumab-Indication-in-Metastatic-Small-Cell-Lung-Cancer-in-the-US-2021.pdf
- Toposar. Prescribing information. Teva Parenteral Medicines, Inc; 2017. Updated April 30, 2017. Accessed May 13, 2021. https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=c9080cf5-4fc3-4cf9-a241-6e40a6fddc75
- Rudin CM, Awad MM, Navarro A, et al. KEYNOTE-604: pembrolizumab (pembro) or placebo plus etoposide and platinum (EP) as first-line therapy for extensive-stage (ES) small-cell lung cancer (SCLC). J Clin Oncol. 2020;38(15):9001-9001. doi:10.1200/JCO.2020.38.15_suppl.9001
- Rudin CM, Awad MM, Navarro A, et al. Pembrolizumab or placebo plus etoposide and platinum as first-line therapy for extensive-stage small-cell lung cancer: randomized, double-blind, phase III KEYNOTE-604 Study. J Clin Oncol. 2020;38(21):2369-2379. doi:10.1200/JCO.20.00793
