Discussing Survivorship in Head and Neck Cancer
Kristie L. Kahl: Can you discuss some of the long-term side effects that patients might experience from either their disease itself or its treatment?
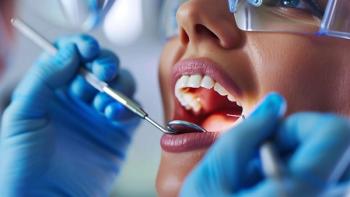
Dr. Michael Moore: There are a lot of them. I think head and neck cancer really affects part of the body that's so central to our day-to-day lives. And I think it can be understated on how important dealing with these treatment-related side effects are. So if you think about it, if you're doing treatment with the common treatments, either surgery or radiation therapy and adding potentially with that chemotherapy for surgery, a lot of it depends on what had to be removed and or rebuilt with surgery. So it can impact, for example, speech and swallowing, it can give the change in appearance. Sometimes it can make it difficult to open and close the mouth. But I think many of the real lingering and troublesome long-term side effects also are centered around after you've had what's called external beam radiation therapy. So that can have an impact on things like the saliva production, it can also impair the ability to care for your teeth well. So without having the regular saliva and the normal dynamic within the mouth, you can get a lot of problems with cavities within the teeth or potentially even damage to the jaw bone itself. And then that treatment also can cause some stiffening in the muscles of the back of the mouth and the throat swallowing more difficult even in the absence of surgery. Also can affect your taste buds itself. As I mentioned, with the saliva going down you can get real problems with constant dry mouth and frequently needing to drink water. They can also have a long-lasting impact on sleep. So whether it's insomnia and difficulty falling asleep, both from physical issues related to their treatment, or also just anxiety and depression related to their cancer care, all those can be really a big a big factor and those who have been fortunate enough to survive that cancer.
Kristie L. Kahl: With all of those long-term effects, is there palliative care? And can you discuss what that is – sometimes people confuse this with hospice?
Dr. Michael Moore: Yeah, I think it's a great point. Palliative care is not the same as hospice. Hospice can be a component of care in instances where cancer is incurable, and in the very end stages of life, but palliative care essentially focuses on how can we optimize the quality of life, and that centers around dealing with treatment-related side effects, pain control, for example, in people who have chronic pain, but it can also deal with things like eating and drinking, recovery and working on symptom management. All those things can go hand-in-shand with cancer treatment. So, it does not mean that you're choosing one or the other. I very frequently will get our palliative care team involved in the care of patients who are going at it with the goal of curing their cancer. And they can be a very important component of that recovery. After the treatment, whether it's surgery and or radiation therapy, they can really be instrumental in optimizing the quality of life and also helping out with things like logistics of getting to and from treatment and any negative impact that could have one either themselves or their caregivers.
Kristie L. Kahl: Can you talk about the fear of recurrence and why patients experienc this, in particular in head and neck cancer?
Dr. Michael Moore: I think it comes hand-in-hand with almost any type of cancer. And I've had friends, I think we all have friends and family members, who have been affected by it. I think it's what consumes much of their day-to-day existence. They're very happy when you hopefully can relay some good news that their cancer looks to be cured or there's no evidence of any remaining cancer. But that only lasts about as long as the next scan or the next doctor's visit, because there's always a concern (the cancer) will come back.
The other challenge is the treatment itself, which results in many of the symptoms that we talked about. And those can often be very similar to what you would experience if the cancer was coming back: a chronic sore throat, difficulty swallowing, things like that can all very much mimic it. And when you take that into account and the fact of all that they went through to get there, they worry of the cancer coming back, I think is that much more significant.
Kristie L. Kahl: Can you also discuss scanxiety?
Dr. Michael Moore: It's basically just what the name implies. When we see patients back after cancer treatment, we'll do regular history and physical exam, we see them in person, we do an exam, to make sure that cancer itself is gone. But as a part of that, we oftentimes will also do different imaging studies to look at areas either under the surface or areas that can't be seen as well just on physical exam, or in other parts of the body. So, for example, head and neck cancer, one of the other main places that we worry about is the lungs, making sure the cancer hasn't spread there. And the only way we'll know whether those areas are affected, especially if it's early in disease, is that they show up on a scan. And so yeah, I had a friend of mine who unfortunately passed away from recurrent cancer and he was a head and neck cancer specialist. And he always said it's changed the entire way that he interacts with patients about this. If they come in and they've had a scan recently, the first thing he does is talk to them that he knows that they're not going to hear anything else that you tell them you want and whether it's good, bad or indifferent. You want to delicately relay that information and then you can work from there because it's really so important because it allows them to where they stand with all the information we have available to us. And I think with that, I try, as much as I can, keep patients on an even keel, don't get too high, don't get too low. We have some good news, but the goal is to proceed with cautious optimism, is typically the way I refer to it, because you want to make sure you keep a level head and making sure we've got the eye on the long-term prize of getting this cancer gone once and for all.
Kristie L. Kahl: Are there resources available for patients to go to that can help them either through these long-term effects or the psychosocial aspects of a head and neck cancer diagnosis?
Dr. Michael Moore: I found that I can talk until I'm blue in the face, and it's not going to really hit home or capture things nearly as well as either talking to peers or actually interfacing with some of the outstanding support and advocacy groups that are available around the country. There are resources online, with different online support communities. The Head and Neck Cancer Alliance I feel is a great organization that really tries to capture the whole gamut, everything from early detection and prevention of cancer to supporting people during the course of treatment. There are many others, though, so Support for People with Oral Head and Neck Cancer is another one, the Oral Cancer Foundation, the Thyroid in Head and Neck Cancer Foundation and many others are great resources for people to go to. And as a result, you can go there, you can not only learn from the materials they have available, but there are different online support opportunities that you can get involved with. There are mentorship programs where around the time of diagnosis, you can get paired with somebody who actually has the same type of cancer that maybe you did, and so it'd be a great resource to talk to during and after treatment as well.