FDA Approvals From Winter 2023 You May Have Missed
Here’s a look back at the cancer drugs that gained FDA approval in the winter of 2023.
New drugs are constantly being studied and developed to improve outcomes for patients with cancer. This winter, we’ve had multiple new therapies introduced into the United States market, for both blood cancers and solid tumors alike.
This winter, the FDA approved multiple new therapies for both solid tumors and blood cancers.
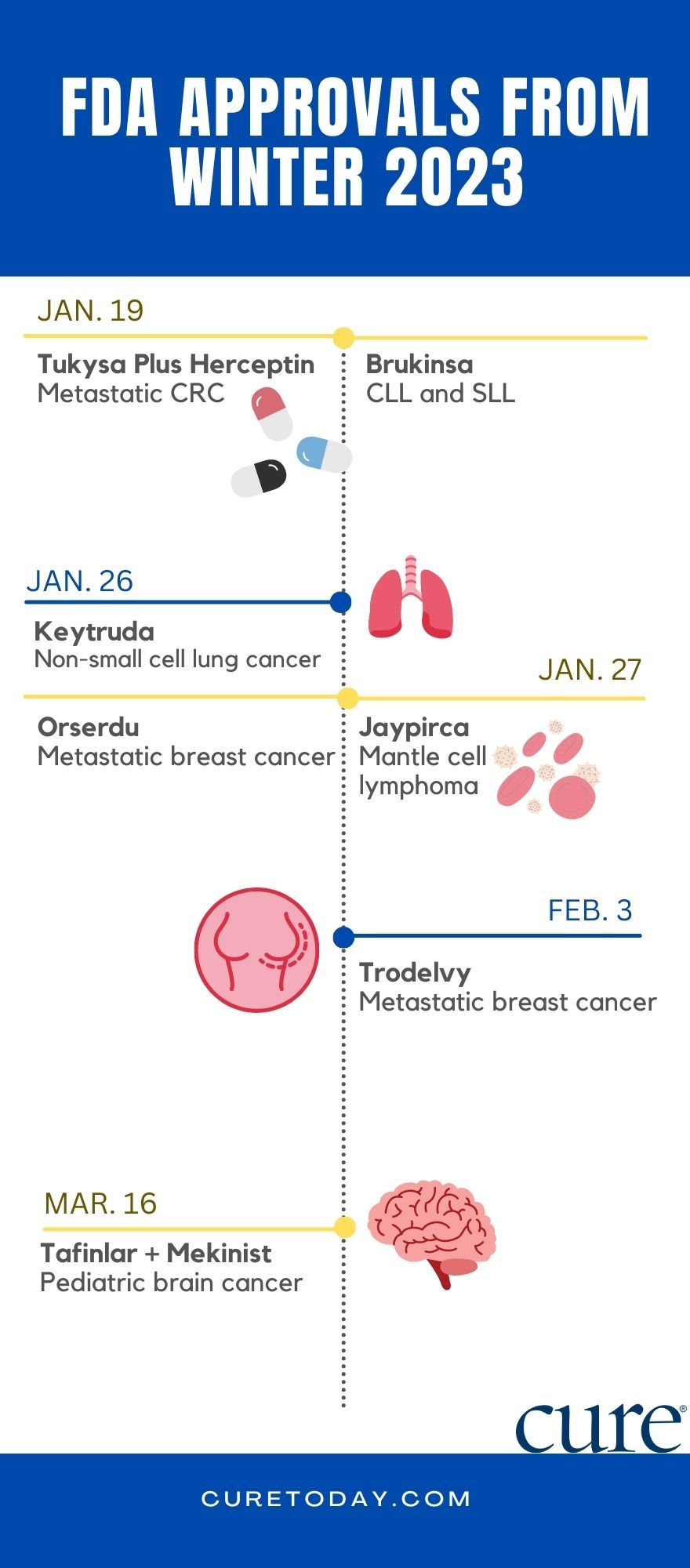
Tukysa Plus Herceptin for Metastatic Colorectal Cancer
On Jan. 19, the FDA approved Tukysa (tucatinib) plus Herceptin (Trastuzumab) for patients with HER2-positive metastatic colorectal cancer. According to Dr. Richard Goldberg from Fight CRC, HER2 mutations occur in about 5-7% of patients with advanced colorectal cancer and, “the most important conversation that patients should have with their provider is having their tumors analyzed using one of the many commercial or institutional panels for looking at driver mutations in tumors.”
The January FDA approval of Brukinsa for chronic lymphocytic leukemia (CLL) and small lymphocytic leukemia (SLL) was based on findings from two clinical trials — SEQUOIA and ALPINE — which showed that Brukinsa tended to improve outcomes and response rates over other therapies for this patient population.
Jaypirca for Relapsed/Refractory Mantle Cell Lymphoma
Also in the blood cancer space, Jaypirca (pirtobrutinib) was approved in late January for the treatment of patients with relapsed/refractory mantle cell lymphoma, who underwent two or more prior lines of therapy. The BRUIN trial that led to the drug’s approval showed that 50% of patients saw their disease shrink due to Jaypirca treatment, and 13% had their disease completely disappear — a metric known as a complete response.
Adjuvant Keytruda for Lung Cancer
The FDA approved, Keytruda (pembrolizumab) for the post-surgical (adjuvant) treatment of patients with stage 1B, 2 or 3A non-small cell lung cancer after a trial showed that the immunotherapy drug improved disease-free survival (time after treatment when a patient survives without any signs or symptoms of the disease) over placebo, something Dr. Roy S. Herbst of Yale Cancer Center called “another form of insurance” to keep lung cancer from returning after surgery.
Trodelvy for HER2-Negative, HR-Positive Breast Cancer
In February, the FDA approved Trodelvy (sacituzumab govitecan-hziy) for patients with locally advanced or metastatic HR-positive, HER2-negative breast cancer that is not eligible to be removed via surgery. The approval is a welcomed one for this patient population, whose disease will often stop responding to prior endocrine-based therapies, explained Dr. Hope S. Rugo, from the UCSF Helen Diller Family Comprehensive Cancer Center.
Orserdu for ER-Positive, HER2-Negative Advanced/Metastatic Breast Cancer
For patients with pretreated advanced or metastatic ER-positive, HER2-negative breast cancer that harbors an ESR1 mutation, the FDA approved Orserdu (elacestrant), based on findings from the EMERALD trial, which showed that patients lived longer before their disease worsened — a statistic called “progression-free survival” — when given Orserdu compared with those who received fulvestrant or another aromatase inhibitor.
Tafinlar Plus Mekinist for Pediatric Brain Tumors
Most recently, the FDA approved Tafinlar (dabrafenib) plus Mekinist (trametinib) for the firstline treatment of children with BRAF V600E-mutant low-grade gliomas, marking the first systemic therapy approved for this patient population. “This has the potential to change the way health care providers treat these pediatric patients, offering a significant advancement compared to chemotherapy,” Dr. Roger Parker, of the Center for Neurosciences and Behavioral Medicine at Children’s National Hospital said.
For more news on cancer updates, research and education, don’t forget to subscribe to CURE®’s newsletters here.