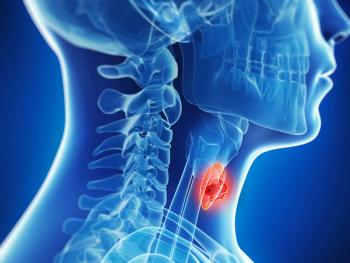
Radioiodine Therapy for Differentiated Thyroid Cancer Following Surgery
Expert perspectives on the process of surgery and radiation therapy used for less severe cases of differentiated thyroid cancer.
Episodes in this series

Transcript:
Bryan McIver, MD: The key message I want to convey is that we have to meet the patient where the patient is. We have to meet their needs, and not every patient is going to benefit from a support group. Not every patient is as resistant as Jim and Molly are and shoulder the burden themselves. They make them pretty tough out there in western Massachusetts. It’s important to provide whatever resources are necessary to help our patients along this journey and tailor the resources we allocate and tailor the treatments to the individual needs of the patient. Something that’s been very clear over the last decade is that treating thyroid cancer is very subtle and nuanced. It has to be tailored to the specific needs of the specific patient with that specific disease. The cookie-cutter approach is no longer acceptable in this disease.
We have to get away from the idea that if everybody gets total removal of the thyroid, doses of radioactive iodine, and then TSH suppression with thyroid hormone, then they’re going to do fine; that’s the cookie cutter. Nowadays, we’re much more selective about how extensive the surgery needs to be. We’re more nuanced about the decision to use or not use radioactive iodine. We are more careful about getting the thyroid hormone levels right. To the point of this presentation, we also need to understand the available treatments that go beyond standard-of-care, previously available treatments and move into targeted therapies and tyrosine kinase therapies, where even more information and understanding of the disease process is critical to allow us to make the right decisions and help our patients survive with high quality of life.
Lori Wirth, MD: Bryan, that’s a perfect segue to talk a little more about the treatment options for patients with differentiated thyroid cancer. Maybe it would make sense for us to talk first about when there’s a role for treatment with radioactive iodine in differentiated thyroid cancer.
Bryan McIver, MD: I’ve believed for my entire career that we should be selective in our use of radioactive iodine. Radioactive iodine is a useful tool because differentiated thyroid cancer, of various types, is capable of absorbing iodine. It’s 1 of the basic functions of the thyroid cells from which these cancers arise. Many of the cancers are capable of absorbing that iodine. If we put into the body radioactive versions of the iodine, the radioactivity is absorbed with the iodine and is held in the thyroid gland. It has a chance then to kill those thyroid cancer cells. We can do that only after the entire thyroid has been removed, so surgery comes first, followed by the radioactive iodine.
There’s good evidence, though not perfect quality, that patients with well-differentiated thyroid cancer that has spread beyond the neck—especially in young people with capillary thyroid cancer with disease of the lung, the most common site for it to spread—that radioactive iodine can batter that disease and push it into total or partial remission. Coupled with appropriate use of thyroid hormone, many young patients with widespread disease live for decades and are often free of disease decades later.
It’s less clear whether there’s a role for radioactive iodine is in treating patients with lymph node disease, because there’s a lack of evidence about how effectively it works. Shame on us as physicians and endocrinologists for failing over the years to do the science necessary to prove when this treatment is really helpful. Certainly, we have to recognize that even with the garden variety “good” thyroid cancers, the recurrence rate can be as high as 20% to 30% when it involves lymph nodes in the side of the neck. Even after great surgery, we have to recognize the high risk of recurrence and do what we can to lower that risk of future recurrence. Radioactive iodine still plays a role in patients with disease contained in the neck, but where the lymph nodes have been involved—especially if those lymph nodes are numerous or bulky—we typically follow with the dose of radioactive iodine.
Radioactive iodine is not the magic eraser we used to think it was. It used to be thought that the patient would receive 1 dose of radioactive iodine and live forever, or 2 doses if the patient had a difficult disease, but that it worked in pretty much everybody. Now we recognize that although it’s a useful tool, it’s far from a guarantee that you’re going to eliminate that cancer. Jim Lesniak has described his experience of cancer that keeps on coming back despite having had radioactive iodine. That indicates that his disease is either not concentrating the iodine or not responding to the radiation, or both. That’s where some of these more advanced therapies and newer therapies come into play.
Lori Wirth, MD: In patients who have had thyroidectomy and then host surgical dose of radioactive iodine, how do you follow them?
Bryan McIver, MD: In general, we follow patients with a combination of appropriate scans and blood work. One nice thing about differentiated thyroid cancer is that it usually produces a protein called thyroglobulin. Thyroglobulin in the blood stream indicates the presence of thyroid tissue. If I have a patient who has had their thyroid removed and had a dose of radioactive iodine, I expect the thyroglobulin to be 0. If it’s not 0, then we may have a problem. Sometimes it’s remnant thyroid tissue, but sometimes it’s leftover cancer. When I go back and monitor the thyroglobulin at increasing intervals, I start 3 to 6 months after the surgery and then at least once a year thereafter, but usually in that first couple of years it’s a little more often.
If the thyroglobulin is undetectable, then we can relax and begin to spread out the intervals until we’re on a once-a-year visit. For somebody who appears to be in remission, we follow that person with an ultrasound scan for the lymph nodes—the most common site for that disease to recur—and thyroglobulin to monitor the activity of the tumor as a whole.
For patients with more advanced disease, bulky lymph nodes, or invasive disease, or in situations where that thyroglobulin doesn’t drop to 0, then we can go hunting for the presence of that disease. We initially use the radioactive iodine as a scanning modality. It’s not uncommon for that to be negative but still with evidence of disease progressing. Then we turn over to use traditional methodology, like a CT scan.
What’s really important, though, is that we have to understand the biology of the cancer. I mentioned earlier in the discussion that the papillary thyroid cancer usually spreads to lymph nodes and then to the lung. Follicular thyroid cancer invades and spreads to bone, so we have to understand the cancer itself. Increasingly, we’re understanding—based not just on the pathology report but on the genetic profile of the cancer—exactly what pattern the disease is going to spread. That allows us to predict where that recurrence is going to be and use appropriate scans to identify the disease.
Transcript edited for clarity.